Peyronie's Disease Treatment Options

Peyronie’s Treatment Curvature Can Be Corrected.
Detailed Testing Reveals the Exact Status of Your Case
Our Doctors Measure Improvement as You Heal
Healing Peyronie’s Disease is Easy as 1,2,3 with the latest treatment options that are effective in healing and correcting the curvature.
After booking your doctor’s appointment, the first step is your new Peyronie’s patient visit.
Our doctors want to know your symptoms, if you’ve already been diagnosed with Peyronie’s disease, any prior treatment methods you already tried, the degree of visible curve you encounter upon erection, and how long you’ve been dealing with plaque and curvature issues.
Additionally, it’s helpful if you take photographs of your penis when erect and bring them with you to your first consultation appointment.
Next, we’ll take steps to create a comprehensive picture of the amount of plaque build-up within your penis and analyze any other issues that might be hindering your penile performance or pain.
This “picture” is produced from ultrasound imagery – you’ll be able to confirm your progress from treatment through the process: this isn’t a guessing game.
With this data in hand, we’ll be able to create a customized healing roadmap for your condition.
Peyronies Disease: What is it?
Listed below are common symptoms associated with Peyronie’s Disease: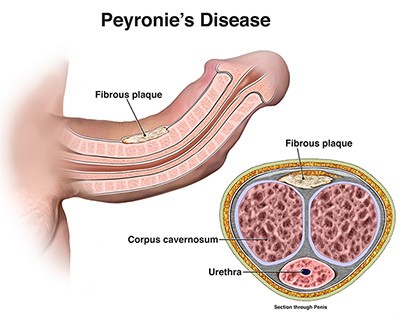
- Plaque Build-up – Plaque, and/or scar tissue, is usually felt underneath the skin of the penis. Lumps are sometimes felt.
- Significant Penis Curvature – Depending on where the plaque build-up is – the penis may be curved to the side, downward, upwards – even multiple directions.
- Erectile Dysfunction (ED)– Men with Peyronie’s often face difficulty in obtaining and/or maintaining an erection.
- Penis Shortening – Over time, men often experience a reduction in penis length, if left untreated.
Pain – The majority of patients find that erections are painful. Pain often occurs during orgasm, as well
Ask About the Peyronie’s Treatment to Correct Penile Curvature
Traditional Treatments
Before the latest Peyronie’s treatment solutions,
Nothing Really Worked
Until now, “no medical therapy has been proven effective for the treatment of Peyronie’s disease[1].”
“Surgical treatment may be an option for some patients, although complications as well as loss of penile length are common outcomes”[2].
The latest treatments and innovations are available at Morganstern Health. A wide variety of treatments have been used over the years in an attempt to arrest the pain and symptoms associated with Peyronie’s Disease with limited success. These treatments include including: Radiation, Verapamil, Collagenase (Xiaflex), Interferon, Traction Devices, Iontophoresis, Surgery, Implants, plus varied Topical Applications, Vitamin E and Herbal Remedies.
[1] Urology Times: March 1, 2012: Outcomes of Peyronie’s surgery worsen over time
[2] Urology Times: March 1, 2012: Outcomes of Peyronie’s surgery worsen over time
Request Information on Peyronie’s Medical Treatment
If the form doesn’t appear above, click here to open it in a new window.
Other Recognized Peyronie’s Disease Treatments
Oral Medications
Oral vitamin E: An antioxidant that is a popular treatment for acute stage Peyronie’s disease because of its mild side effects and low cost. While studies as far back as 1948 have demonstrated decreases in penile curvature and plaque size from vitamin E treatment, most of these studies have not used placebo controls. Those few studies of vitamin E that have included a placebo treatment group have demonstrated that vitamin E does not appear to give better results than the placebo, which calls into question whether or not vitamin E is an effective treatment.
Potassium amino-benzoate: Also known as Potaba. Small placebo-controlled studies have shown that this B-complex substance popular in Central Europe yields some benefits with respect to plaque size, but not curvature. Unfortunately, it is somewhat expensive and use of the medication requires taking 24 pills a day for three to six months. This medication has also been associated with a high rate of stomach upset, which leads many men to stop taking it.
Tamoxifen: This non-steroidal, anti-estrogen medication has been used in the treatment of desmoid tumors, a condition with properties similar to Peyronie’s disease. Unfortunately, placebo-controlled trials of this drug are rare and the few that have been conducted have not shown that Tamoxifen is better than placebo.
Colchicine: An anti-inflammatory agent that decreases collagen development. Colchicine has been shown to be slightly beneficial in a few small, uncontrolled studies. Many patients taking colchicine over the long term develop gastrointestinal problems and must discontinue the drug early in treatment. It has not been proven to be superior to placebo.
Carnitine: An antioxidant medication that is designed to reduce inflammation and thereby decrease abnormal wound healing. Like many other Peyronie’s therapies, uncontrolled trials have demonstrated some benefit using this treatment but a recent controlled trial has not demonstrated it to be superior to placebo.[/fusion_text][fusion_text]Penile Injections
Injecting a drug directly into the plaque of Peyronie’s disease is a common form of treatment for Peyronie’s.
Two drug platforms have been used – each with limited success:
Verapamil
Verapamil is one of the most popular treatments, its injected directly into the plaque built up in the penis. Although it helps to soften this plaque in hopes of breaking it down – its just not strong enough to effectively treat anything but the mildest beginning cases.
Xiaflex
Collagenase is another popular injectable method that’s now usually done with the popular medication Xiaflex. Xiaflex 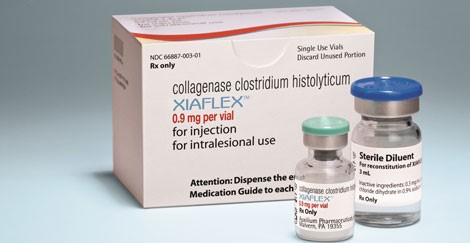 is used only when the original curve is greater than 30 degrees – since that’s when major insurers will provide reimbursement as the drug is very expensive.
is used only when the original curve is greater than 30 degrees – since that’s when major insurers will provide reimbursement as the drug is very expensive.
The launch of Xiaflex as a possible solution for Peyronies caused a stir during its launch in 2012. But a key researcher in the tests and trials that supported its introduction was more low-key. The results “are not overwhelming and dramatic,” said Dr. Culley C. Carson III, a professor of urology at the University of North Carolina and an investigator in the trial. But, he added, “it’s a major advantage over what we have now, which is nothing.”
Xiaflex faces a number of important limitations:
- It doesn’t remove the built-up plaque. Thus, even if Xiaflex is successful in unbending the curve of Peyronie’s disease through scar tissue dissolution, the patient will often still suffer from a shorter, morphed penis full of varied plaque.
- It can’t be injected into calcified plaque – Xiaflex is unable to penetrate the calcified plaque commonly found in patients with a curve in excess of thirty degrees. If its used in such cases, the powerful acidic solution usually drains around that impenetrable barrier and seeps into the corpus cavernosum – the sponge-like functional sector of the penis responsible for erection. This seepage can result in permanent impotence for the patient.
- It can’t be used to treat the underside of the penis – If the source of the bed is located on the underside of the penis, Xiaflex is not indicated for use because of the likelihood of chemically damaging the urethra.
Surgical Treatment of Peyronie’s Disease
Surgery for Peyronie’s is currently only indicated in the chronic, stable state of the disease in patients with a degree of curvature that does not allow for sexual intercourse and/or causes pain.
Surgery is used to completely remove the buildup of plaque within the penis but this is a last resort method. Peyronie’s Disease Surgery can have serious complications and side effects such as shortening of the penis and ED. Implants are another method to try and fix Peyronie’s Disease that involved surgery. Once again the complications and side effects are great and men should consider every other option before going down this road.
Long Term Peyronie’s Surgical Outcomes Less Positive Than Expected
A first-ever retrospective study on the long term efficaciousness of Peyronie’s disease completed in 2012 offered a dismal view on the success of such surgery with healing Peyronies. According to a recent retrospective study published by Florian Wimpissinger, MD, of the department of urology at Rudolfstiftung Hospital in Vienna, Austria in 2012 regarding the long term outcomes associated with PD surgery, results are anything but ideal.
After a mean of 9.3 years, the recurrence of postoperative curvature had increased from 0% after a mean of 38 months (18–73 months) to 23.7%, post-op erectile dysfunction increased from 3.0% to 39.5%, penile shortening from 0.0% to 65.8%, and impairment of penile sensitivity from 3% to 31.4%.
“We saw that results tend to worsen with time,” said Dr. Wimpissinger, who presented the study results at the 2011 European Association of Urology annual congress in Vienna. “Since these results were much better during the first months or few years following surgery, it can be assumed that all these aspects are caused by the chronic/recurring nature of PD,” Dr. Wimpissinger said.
“From what we found after many years of follow-up, all published data on the results of PD surgery have to be interpreted in a different light,” said Dr. Wimpissinger.
In other words?
Long-term results from surgery indicate the condition returns and becomes equally debilitating and painful.
We have the technology that changes all this.
Based upon recent results from over 400 patients at our flagship facility in Atlanta, our doctors witnessed a 100% success rate eliminating fibrous and calcified plaque associated with Peyronie’s amongst compliant patients. All compliant patients saw significant or complete reduction in the unsightly curve associated with Peyronie’s Disease.
Our Philosophy
Our clinic is focused on finding a cure for Peyronie’s Disease. After more than two decades of research and development, we’ve achieved many major milestones in pursuit of our purpose, including:
- We identified the underlying epidemiology of Peyronie’s.
- Our research identified six Peyronie’s Accelerators that need to be regulated and optimized to treat the disease.
- Our patented therapeutic uses pulsated gas injections to penetrate Peyronie’s fibrous plaques, allowing medications to breakdown fibrosis without surgery.
- Our new therapy algorithm takes into account all variables of a Peyronie’s case, such as plaque size, density, and position, as well as health factor rating and the state of each Peyronie’s Accelerator. This will assist future clinicians in treating cases.
Earlier in our Peyronie’s technology development, we were unable to restore the original size of the penis following the removal of Peyronie’s plaques, therefore we developed unique approaches for cosmetic urology (penis augmentation). Since then, we’ve learned ways to restore lost size from Peyronie’s during therapeutic treatments, but our cosmetic urology platform, led by renowned reconstructive urologist Kenneth J. Carney, MD, PHARM, FACS, has been highly successful. Our cosmetic platform has provided the principal funding for our Peyronie’s research.
We are now developing technology to accelerate the progression of obstinate Peyronie’s cases using enhanced techniques and innovative medications. We have initiated negotiations to partner with a multinational pharmaceutical platform to fund our FDA approvals and help ensure the ExoSurge breakthrough is available internationally in the coming years.
